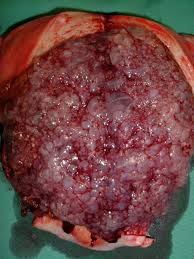
 Hydatidiform mole is an abnormal pregnancy in which almost all villi chorialis hydropic degeneration. Layman's terms: "pregnant wine." Happened hydropic degeneration of the trophoblast tissue in younger gestational age. B-hCG levels rose very high, causing the symptoms arise young pregnancy excessive.
Hydatidiform mole is an abnormal pregnancy in which almost all villi chorialis hydropic degeneration. Layman's terms: "pregnant wine." Happened hydropic degeneration of the trophoblast tissue in younger gestational age. B-hCG levels rose very high, causing the symptoms arise young pregnancy excessive.
Division [-] Classical hydatidiform mole / complete: there is no fetus or fetal body parts. Histological characteristics, there is a picture of trophoblastic proliferation, hydropic degeneration of villi chorialis and reduced vascular / capillary in the stroma. Often accompanied by the formation of lutein cysts (25-30%). [-] Partial hydatidiform mole / incomplete: there is a fetus or fetal body parts. Histological characteristics, there is a healthy placental tissue and the fetus. Preview villi only focal edema and proliferation of trophoblast only mild and limited to the syncytiotrophoblast layer. Fetal development is hampered due to chromosomal abnormalities and usually die in the first trimester.
Symptoms [-] Bleeding: hydatidiform pressure to the uterine wall [-] Young pregnancy symptoms of excess: hyperemesis, hyperthyroidism, preeclampsia, anemia
Pathogenesis [-] B-hCG increased - increased activity of the ovaries (cystic ovaries) - high estrogen effect hyperthyroidism of activity of B-hCG is high. [-] The theory of Acosta-Sison: protein deficiency. [-] Cytogenetics: complete hydatidiform mole comes from the paternal genome (genotype 46 xx frequently, 46 xy rare, but 46 of them come from reduplication xx haploid sperm and without the chromosome of the ovum). Partial mole has 69 chromosomes consist of haploid chromosome 2 paternal and 1 maternal haploid (triploid, 69 or 69 xxx XxY of a haploid ovum and the other reduplication of one paternal haploid sperm or fertilization dispermia).
High risk groups [-] Less than 20 years of age [-] Less socioeconomically [-] The number of high parity [-] A history of previous molar pregnancies
Diagnostic hydatidiform mole [-] Anamnesis: no pregnancy symptoms and signs of excessive youth pregnancy, recurrent vaginal bleeding brown and sometimes tend to like a bubbly foam. [-] Physical examination: the classic mole, enlarged uterus exceeds the appropriate size for gestational age, no palpable part of the fetus, no fetal heart sounds. Sonde stem test (Acosta-Sison / Hanifa) there is no conception of mass resistance. In partial mole, symptoms such as a missed abortion, the uterus is smaller than the pregnancy. [-] Investigation: if possible, check the quantitative B-hCG and ultrasound. Ultrasound images such as snow storms (Snowflake / snowstorm-like appearance). Chest radiograph and T4 T3 levels is recommended. Examination of B-hCG: [+] Biological: Gaili Mainnini, Friedman [+] Immunologic tests: no quantitative [+] Radioimunoassay: quantitative Hyperthyroidism: B-hCG> 300,000 mIU / ml - affect thyrotropin receptor - activity of thyroid hormones (T3/T4) increases. Symptoms of hyperthyroidism occur in the form of hypertension, tachycardia, tremor, hyperhidrosis, restlessness, emotional instability, diarrhea, vomiting, increased appetite but weight loss and so forth. These symptoms were treated with propylthiouracyl 3 x 100 mg oral propranolol 40-80 mg. Thyroid crisis: uncontrolled hyperthyroidism, accompanied by hyperthermia, convulsions, cardiovascular collapse, toxemia, delirium, decreased consciousness until coma.
Principle handling [-] Note the syndrome that threatens vital functions (respiratory depression, hyperthyroidism / thyrotoxicosis, etc.), ready to resuscitate if the patient's general condition worse. [-] Evacuation of molar tissue: dilatation-curettage with suction (suction) and sharp curettage. Suction to remove most of the molar mass, the rest is cleaned with a curette. It can also do induction. At the time of evacuation, given oxytocin to stimulate uterine contractions and prevent reflux of fluid into the fallopian mole. [-] In women who are not expecting another child may be recommended hysterectomy.
Follow up / post-evacuation of hydatidiform further observation The control of progression into malignant trophoblastic disease (choriocarcinoma) [-] Prophylaxis against malignancies with sitostatica, especially in high-risk group of malignancy. [-] Gynecologic examination and routine quantitative B-hCG every 2 weeks after the evacuation until remission, after remission, remains regularly every 3 months to 1 year. [-] Chest radiograph at the beginning of therapy, repeated if the B-hCG levels persist or increase. [-] Hormonal contraceptives safe for 1 year after remission. We recommend using oral progesterone preparations for 2 years. [-] Counseling patients about the possibility of malignancy
Risk factors for high / bad prognostic [-] B-hCG> 100,000 mIU / ml [-] Bilateral lutein cysts [-] Recurrent hydatidiform
www.dokter-online.org
New Article
Free E-Book
Hydatidiform mole
Diposkan oleh Happy Baby & Kid di 12:51 PM
Label: Hydatidiform mole, mom, Pregnancy, women
